Folliculitis
13 September 2022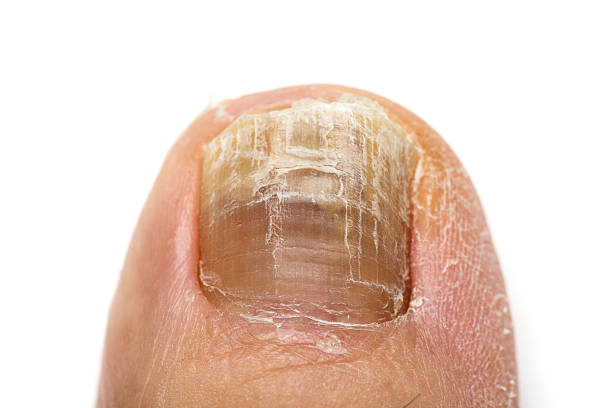
Nail Conditions
13 September 2022Normal hair growth and hair loss occurs in a 3-phase cycle:
- Anagen (2-6 years) – active growth phase; nourishment of hair follicle via blood supply enables hair growth
- Catagen (1-2 weeks) – transition phase; hair follicle detaches from nourishing blood supply
- Telogen (2-4 months) – resting phase; without nourishment, the hair follicle dies and falls out; return to Anagen – hair matrix forms new hair
Abnormal hair loss is usually due to one of the following conditions:
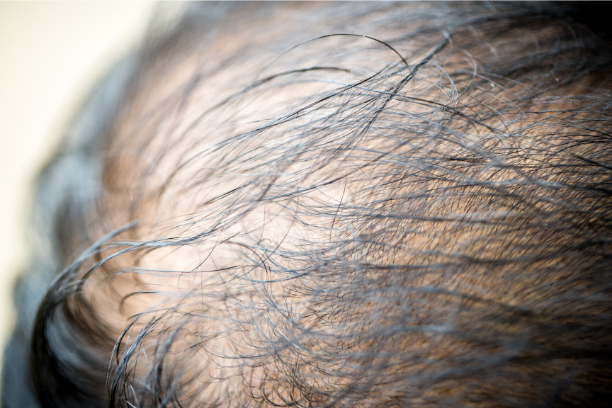
Androgenic Alopecia
Male Pattern Hair Loss (MPHL) is common in men over 70 years old and often younger, and it is hereditary. It is known to be exacerbated by high levels of androgenic hormones in the body. Androgens drive the conversion of thick, lustre ‘terminal’ hairs into fine, wispy ‘vellus’ hairs like those covering the body during childhood. This process is called ‘miniaturisation’.
Research shows that dihydrotestosterone (DHT) is implicated in miniaturisation, and that when these hormone levels are normalised this process can be halted or even reversed. Sub-optimal iron levels can also have an impact on hair growth.
Conventional treatment for MPHL involves taking anti-androgenic drugs suppress your hormones and can have many unwanted side-effects. They can also create drug-dependency to maintain the results because they don’t reduce your natural androgen production.
Female Pattern Hair Loss (FPHL) can occur in women going through hormonal changes like pregnancy and menopause. It can be hereditary but is also driven by high levels of androgenic hormones in the body. Androgens drive the conversion of thick, lustre ‘terminal’ hairs into fine, wispy ‘vellus’ hairs like those covering the body during childhood. This process is called ‘miniaturisation’.
Signs of Hyperandrogenism in women are weight gain (especially around the middle), hirsutism, menstrual disturbances, acne, increasing muscle mass in active people and enlarged genitalia.
Research shows that dihydrotestosterone (DHT) is implicated in miniaturisation of hair follicles, and that when these hormone levels are normalised this process can be halted or even reversed. Sub-optimal iron levels can also have an impact on hair growth.
Conventional treatment for FPHL involves taking anti-androgenic drugs suppress your hormones and can have many unwanted side-effects. This treatment can also create drug-dependency to maintain the results because they don’t reduce your natural androgen production.
Synthetic hormones are often given to women in the form of the Oral Contraceptive Pill (OCP) to address hormonal deficiencies. Taking synthetic hormones reduces your body’s natural production of these same hormones. Your endocrine glands won’t produce as much of these hormones if there is an external source available.
The role of androgens
Aromatisation: High androgens often result in high estrogen in both men and women because they ‘aromatise’ testosterone into estrogen. Aromatisation is the process that converts testosterone into estrogen. This is a natural process your body goes through to maintain homeostasis. The reason that this process is called aromatisation is because it is named after the chief enzyme involved in the conversion – aromatase. While aromatisation mostly occurs in the male body, it also occurs naturally in the female body as well if testosterone levels become out of balance.
Progesterone: Progesterone keeps 5-alpha-reductase enzyme levels in check, thereby preventing the conversion of Testosterone to DHT (more potent androgen). Progesterone is known as a female hormone, but males need progesterone to produce testosterone. The adrenal glands and testes in males produce progesterone. Progesterone levels naturally drop in men as they age. Symptoms of low progesterone in men include hair loss, low libido, sexual dysfunction, depression, bone and muscle loss.
Telogen Effluvium
Early and excessive loss of normal club hairs from normal resting follicles in the scalp. Abnormally large numbers of hairs simultaneously enter the telogen phase resulting in diffuse thinning of the hair on the entire scalp.
There is usually a precipitating event. Causes include postpartum, post-febrile, severe infection or chronic disease (HIV, Colitis, Lupus etc.), severe prolonged stress, surgery, hypothyroidism and other endocrinopathies, crash diets (starvation/malnutrition), many medications. Hair loss typically starts 3 months after the precipitating event.
Medications associated with TE: stopping the Oral Contraceptive Pill (OCP), retinoids (like isotretinoin), anticoagulants, anti-thyroid medications, anti-convulsant medications, interferon-α-2b, β-blockers, and heavy metals.
| FPHL vs. CTE | ||
| FPHL | Chronic TE | |
| Distribution | Central portion of scalp and preserved frontal hairline | Generalised |
| Onset | Gradual | Abrupt with a trigger |
| Appearance | Hair Thinning with wide midline parting | Diffuse thinning |
| Hair shedding | Minimal | Prominent |
| Hair pull test | Usually negative | Positive |
| Other history | Family History | Previous major injury or stress |
Hair Pull Test: Gentle hair pull – positive for 2 or more hairs coming away in your hands.
How to perform 60-second times hair count: Comb the hair forward for 60 seconds over cloth of a contrasting colour while dry and before shampooing. Count the hairs lost: 10 hairs normal, more than that is suggestive of Telogen effluvium.
Natural Treatment of Telogen Effluvium depends on the precipitating trigger and/or underlying condition. Lab tests and perhaps HTMA to detect heavy metals will help determine the course of action.
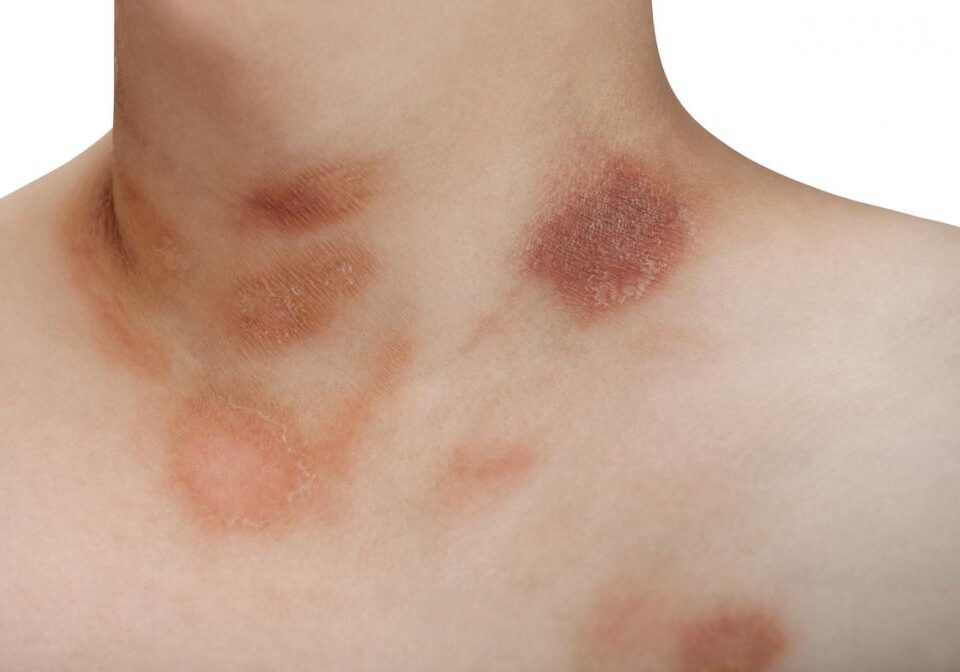
Alopecia Areata
Alopecia areata is a common pattern hair loss caused by a T-cell mediated autoimmune reaction. There are 6 forms of Alopecia areata:
Patchy alopecia areata: one or more roundish patches on scalp or elsewhere on the body (can mimic Tinea Capitis/ringworm)
Persistent patchy alopecia areata: Patches persist over a long time
Alopecia totalis: Hair loss of the entire scalp
Alopecia universalis: Scalp, face (incl. eyebrows and eyelashes), and entire body (incl. pubic hair)
Diffuse alopecia areata: Not as common, diffuse, sudden thinning and loss of hair
Ophiasis: Band shape loss of hair involving occipital area
There may be nail involvement: Nail pitting, trachyonychia, brittle nails, oncholysis, koilonychia, onchomadesis
Physical course
Regrowth and relapse is unpredictable and there is no definite cure. Hair regrowth can happen spontaneously after years of widespread hair loss. Regrown hairs can be grey/white initially and then re-pigment within weeks or months.
Our approach to hair loss
At Auckland Skin Clinic we provide specific supplements and herbal medicines that support hair growth in a safe and effective way. We address the underlying cause of your hair loss condition. We do lab test and hormone tests where appropriate to help tailor your treatment and get the best long-term results.
At Auckland Skin Clinic safe, topical agents are used to soothe the scalp and support healthy hair growth, while underlying environmental and lifestyle triggers are identified and addressed.
At Auckland Skin Clinic, we’re aware that having a hair loss problem can be very frustrating, embarrassing and depressing. We are also aware that it often requires some major effort on your part to change your habits and adopt a healthy lifestyle. We do our best to ensure your emotional well-being is supported throughout this process.