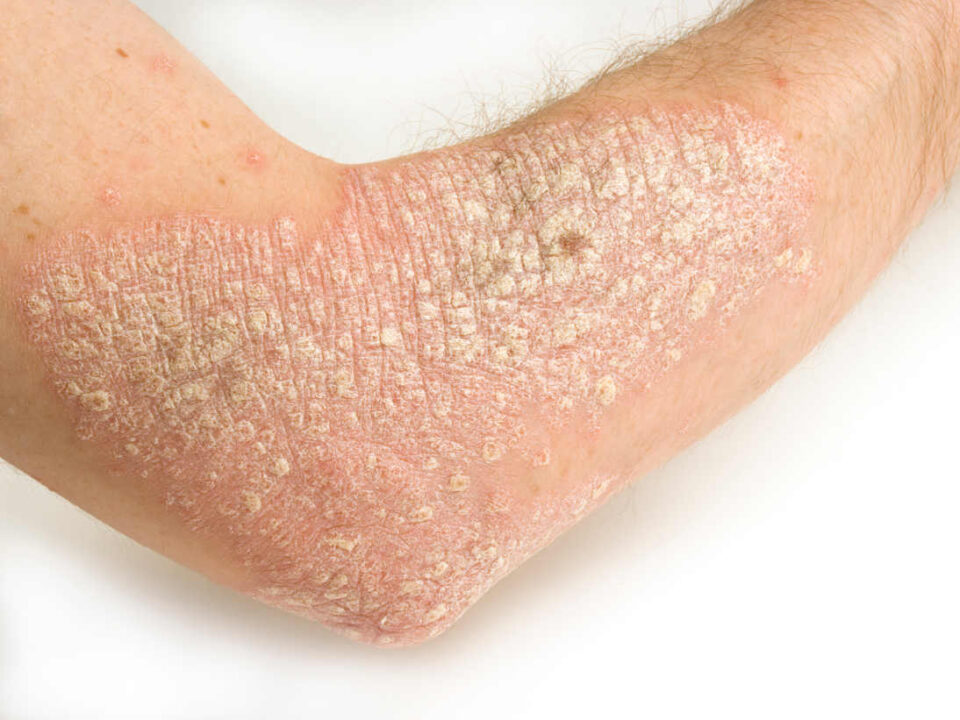
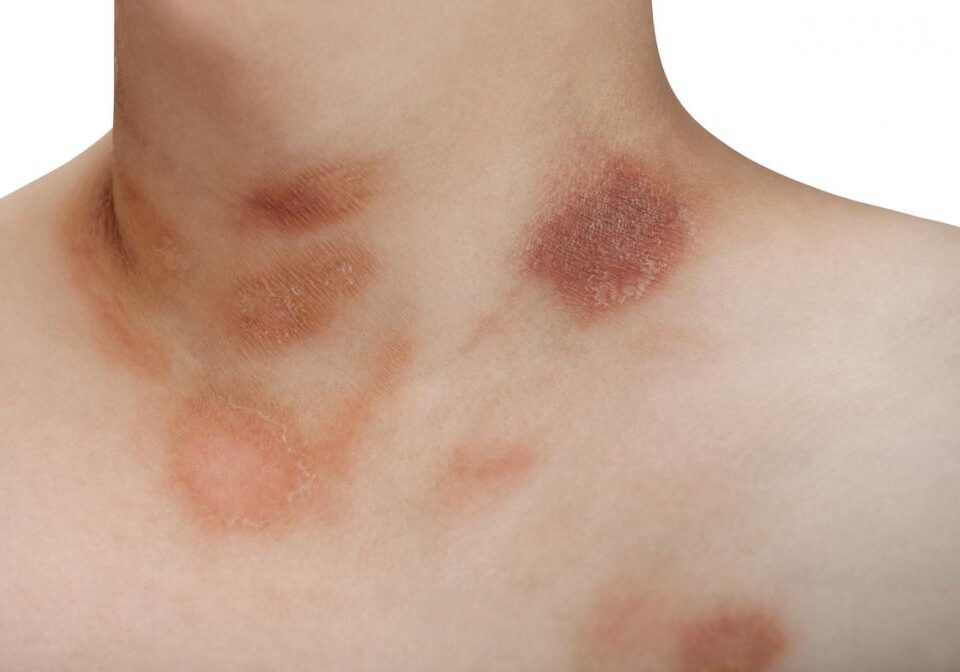
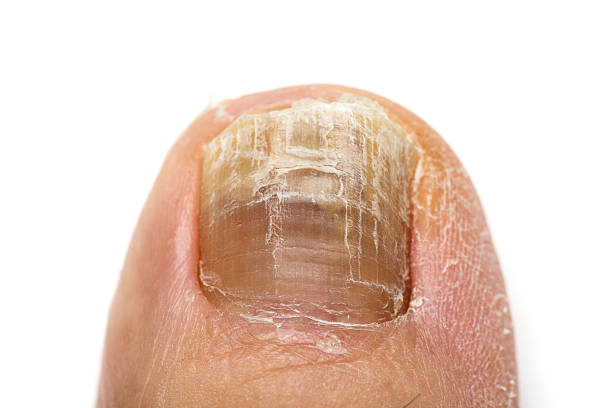
Tinea
13 September 2022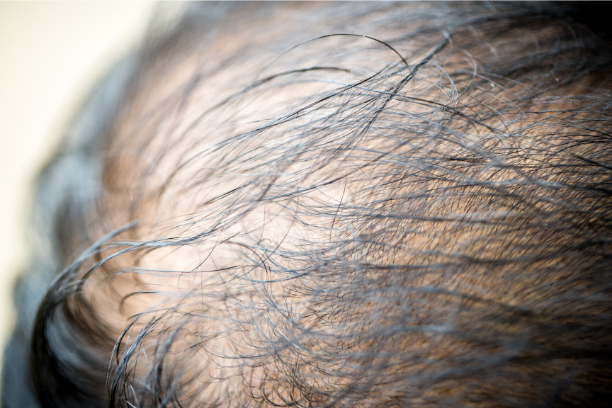
Hair Loss
13 September 2022Folliculitis is characterised by inflammation of hair follicles and can occur anywhere on the body where there is hair. Folliculitis can be triggered by bacterial, fungal or parasitic infection, specific medications, topical agents, immunosuppression disorders, or other inflammatory skin diseases. It typically results in sore, inflamed pustules, similiar to acne.
Types of Folliculitis:
Bacterial folliculitis is infection of the deep hair follicle resulting in a painful boil. It is often caused by Staphylococcus aureus bacteria. Spa pool folliculitis is due to infection with Pseudomonas aeruginosa bacteria. The same bacteria can cause facial eruptions known as Gram negative folliculitis.
Malassezia folliculitis or Pityrosporum folliculitis is caused by Pityrosporum ovale yeast overgrowth, and typically results in an itchy acne-like condition on the upper trunk. Candida albicans can also cause folliculitis in the skin folds or beard area.
Tinea capitis, of the scalp, also known as ringworm, can result in folliculitis as the scalp becomes infected and inflamed.
Viral infection from Herpes simplex virus, Herpes zoster virus (shingles), or Molluscum contagiosum, can result in folliculitis in affected areas of the body.
Parasites such as scabies or hair follicle mite (demodex mites) infestations often provoke folliculitis.
Irritant folliculitis commonly occurs in men and women after shaving, waxing, electrolysis or plucking and may be coupled with ingrown hairs. In the beard are it is known as Pseudofolliculitis barbae.
Our approach
Regardless of the type of folliculitis or the age of onset folliculitis can be painful, can contribute to negative self-image and self-esteem and can be difficult to manage on a day to day basis.
Folliculitis is a multi-factorial condition thus the Integrative Dermatology approach to treating folliculitis is holistic at its essence. Safe, topical agents and cleansers are used to help support healthy skin, while underlying infections, dietary, environmental and lifestyle triggers are identified and addressed.
At Auckland Skin Clinic, we’re aware that having a chronic skin disorder can be very frustrating, embarrassing and depressing. We are also aware that it often requires some major effort on your part to change your habits and adopt a healthy lifestyle. We do our best to ensure your emotional wellbeing is supported throughout this process.